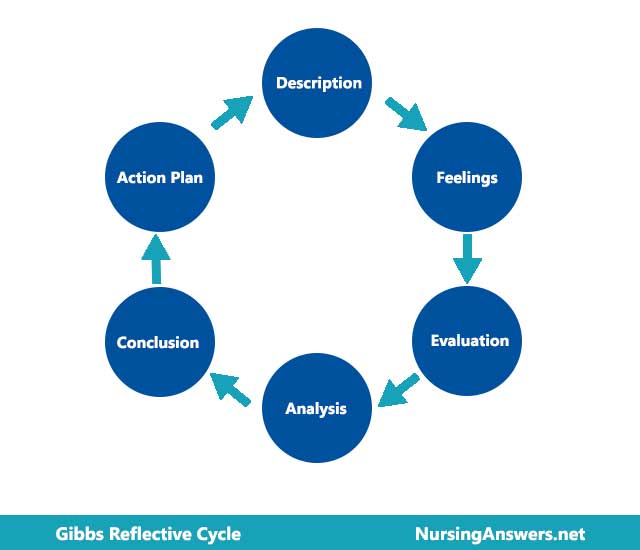
In this essay, I will reflect upon a experience which I had with a patient using the Gibbs cycle of reflection (Gibbs, 1998) to help to signpost my answer and help the reader to read this essay with ease.
Description of the event: During my clinical placement I have encountered a number of patients, each one possessing a unique personality thereby required a slight adaptation of my professional behaviour in order to communicate most effectively with each individual. During one particular placement within my allocated hospital, I encountered a patient who was younger than the patients that I had previous met and conversed with over the previous months. The patient, aged 3 months, attended the clinic with his father regarding his physiotherapy for his Cystic Fibrosis (CF). I was asked to carry out a subjective assessment of the patient however, the setting of this encounter was rather different from the set-up which had been used in the past, and although I had seen patients who were younger in the past, this patient was different as it rapidly became apparent that he had been brought by his father who was unable to speak fluent English and was also unable to understand much English at all.
In the normal situation with young patients, due to the patients young age and the presence of her father, it would be typical to direct most of the questioning towards the patients parents or guardian with whom they attended rather than at the patient himself, despite the necessary inclusion of the patient in the discussion wherever possible. I would then physically assess the patient. However, in this setting, it was very difficult to ask any questions to both the patient or to their parent and instead, most of the information about the health of the patient and their physiotherapeutic interventions which they required was gained from the examination of the patient and not from any information which they provided.
Feelings: Upon reflection, I feel that although, at first the situation did both feel and appear new and challenging, my ability to communicate with the client was not helped by the fact that I was unable to think of a new way to phrase the questions, which I had. In addition, the patient’s father kept looking at the trained physiotherapist (my mentor) for reassurance and guidance with the language being used and thus, this made me also look towards my mentor for help. When my mentor took over the line of questioning, and the conduction of the assessment, his approach was to ask the patients the questions in a loud and slow voice. This appeared to aid the patient’s fathers understanding greatly. I felt, at this point however, that I had let myself and the mentor down, as I was unable to conduct the procedures which I was expecting to and I also felt that I had let the patient down, through my inability to communicate effectively with them.
When examining the patient, my tutor made sure that he looked at the patients father at all times when speaking and also that he used body language to highlight the meaning of what he was saying also. This again, helped the patient’s father to understand the meaning of what was being carried out and what was being said. Visual aids were also used to ensure that the patient’s father understood. For example, when my tutor was asking whether the patient had taken his antibiotics for his CF and what physiotherapy he thought his child required. When asking such questions, he pointed to a prescription on his desk, which helped the father to understand what was being said. This clearly made the difference between the patient not understanding what was being said to gaining an appropriate understanding and being able to answer the questions properly and accordingly.
Evaluation: From this experience I also learnt that in the case of younger patients, particularly babies, it is important to be able to talk to the parents, as the patient themselves would be unable to provide information. This is because when a child has a condition such as CF, it is regularly the parents who will be worried and concerned about this and additionally; it is the parents who deal with the physiotherapy and the treatments, which the child receives. Additionally, it will be the parents of the child who will manage the symptoms that their child has, and conduct the physiotherapeutic interventions on the child until they come of age where this can be continued by the child. In the case of the patient who was not fluent in speaking English, I have noted the importance of speaking both loudly, and slowly and using all the different sorts of body language possible in order to ensure that the patient’s parents were put at ease and were able to comprehend the questions, which were being asked.
Analysis: My experience has taught me that in order to improve my communication skills with patients of different languages, I will need to increase my interaction with a range of patients with different native languages and those who are not fluent in speaking English. This will most likely be achieved through increased exposure to patients within my clinical placement and I will try to ensure that I increase my exposure to individuals of a variety of nationalities wherever possible within my placements. Meeting this patient and his father also highlighted the requirement to adapt not only the language used when asking questions, but also the language tone and the nature of my body language used throughout the assessment.
Conclusion: In conclusion, due to the presence of both the patient (the baby) and his father, not only did this patient encounter bring with it the challenge of the language barrier, but it also brought the experience of needing to integrate multiple people into a conversation without loosing the flow of the conversation. For example, it was clear that there was a need to build a rapport with the patient themselves, despite their young age, in order to put them at ease during their physical, physiological examination. This is important for physiotherapists to establish a good patient rapport, especially with children, in order to make physical assessment easier. This was clear because when the patient first entered the room, he was looking around the room and not smiling very frequently. After being within our company for a small amount of time, and after I had smiled at the patient and looked at him to engage him when speaking to his father it was clear that he felt much more relaxed and comfortable as he began to smile and look at us when we were talking. He was less interested in his surroundings and appeared to be much more at ease.
Action plan: The experience also showed that I must work on my communication skills and my coping strategies in different clinical situations. Thus, in the future, I aim to increase my level of exposure to patients of all ages by attending a variety of physiotherapy clinics and talking to patients. This should help in the development of such skills and make experiences such as this, much easier to manage effectively.
Cite This Work
To export a reference to this article please select a referencing style below:
Related Content
All TagsContent relating to: "gibbs reflective cycle"
Gibbs' Reflective Cycle was developed by Graham Gibbs in 1988 to give structure to learning from experiences. It offers a framework for examining experiences, and given its cyclic nature lends itself particularly well to repeated experiences, allowing you to learn and plan from things that either went well or didn’t go well. It covers 6 stages.
Related Articles